Implant indications
Tooth vs implant
Introduction
As clinicians, we would often find patients with very poor oral health. They had residual dentition which had been damaged by periodontal disease or decay lesions and which could no longer fulfil their functional and aesthetics requirements.
Before dental implants existed, fixed prosthetic solutions relied on natural abutments (provided that they were healthy enough). Now, clinicians and patients have to make their treatment decisions while taking both teeth and implants into consideration. The clinicians’ goal is to improve the quality of life of their patients. With this in mind, decision making is a complex process, and there are many circumstances which need to be taken into account.
“Decision making is a complex process”
When facing a new case, clinicians have to answer the following questions: when are implants better than teeth? Should all teeth be extracted or are there still some which could be used as abutments? Is it possible to use a combined approach utilising both teeth and implants?
All on teeth
When the remaining teeth can be maintained healthily and they are suitably distributed around the arch, tooth-supported reconstructions can provide a predictable solution, even in cases with periodontally reduced abutments. The speaker presented an impressive case which had been treated over 30 years ago involving full-arch prostheses in the upper and lower jaw, supported by five roots each.
The speaker stated that Ante’s law (Ante. 1926) is an old and outdated opinion: it is completely useless in today’s landscape. Since Ante’s law was published, it has been clinically demonstrated that even a reduced periodontium has the capacity to support fixed bridges (Nyman & Ericsson. 1982; Lulic et al. 2007). It has been shown in a number of systematic reviews that the ten-year results of prostheses on teeth with reduced periodontal support were better than those of implants.
“Give teeth a chance”
The speaker said that the eagerness of some clinicians to place dental implants (termed the ‘euphoria for dental implants’) often led to the mutilation of periodontally affected dentitions. They would often extract teeth which could have been used as abutments in order to place implants.
“The patient’s capacity to take care of their teeth is a prerequisite for long-term results”
The speaker concluded his presentation by cautioning the audience: treatment plans should be carefully discussed with patients. Clinicians should also take care to bolster their patients’ motivation for maintenance, since this is a key factor in the therapeutic decision. The patient’s capacity to take care of their teeth is a prerequisite for long-term results and this often demands a change of lifelong habits.
References:
Ante IH. The fundamental principles of abutments. Michigan State Dental Society Bulletin 1926;8:14–23
Lulic M, Brägger U, Lang NP, Zwahlen M, Salvi GE. Ante’s (1926) law revisited: a systematic review on survival rates and complications of fixed dental prostheses (FDPs) on severely reduced periodontal tissue support. Clin Oral Implants Res. 2007 Jun;18 Suppl 3:63–72.
Nyman S, Ericsson I. The capacity of reduced periodontal tissues to support fixed bridgework. J Clin Periodontol. 1982 Sep;9(5):409–14.
All on implants
With a long-term survival rate of 97%, the ‘all-on-implants’ treatment approach has changed a great deal over the years. Some of the improvements which have been made are: less morbidity, quicker treatment, lower costs, less effort required from the patient and a better quality of life during treatment.
But when is ‘all-on-implants’ the treatment of choice? There are some desperate cases where this approach is undoubtedly the best choice. The speaker described an all-on-four approach using tilted implants and immediate restoration. Within hours, this approach can dramatically change the patient’s life and can improve their oral care in the future.
But there are other cases where the answer is ‘maybe’. Sometimes, teeth can be maintained after periodontal treatment.
“Sometimes, teeth can be maintained after periodontal treatment.”
The speaker presented a number of cases where the decision had to be made whether to treat with an all-on-implants approach. One patient (Figures 1–3) had problems in both the upper and lower jaws. The speaker invited the audience to vote on which approach they would choose for restoring the jaws (Figures 4–5).
The speaker then showed the results. They treated with traditional, non-surgical periodontal treatment. To enhance the aesthetic, they worked with composite (Figures 6–10). Due to financial limitations and the patients’ wishes, they did not place implants in either the upper or lower jaw. However, the speaker stated that in the future, they will most likely place two implants in the lower jaw.
The second case presented involved a 66-year-old man who had lost many teeth in the past (Figures 11–14). The radiograph showed root caries in the molar in the upper jaw. In the lower jaw, there was advanced periodontal disease present and vertical defects and apical lesions.
Once again, the speaker invited the audience to vote on how they would restore the jaws (Figures 15–16). He then showed the treatment approach which was undertaken: the teeth were extracted in the upper jaw, and four tilted implants were placed (Figures 17–18). In the lower jaw, they kept all the teeth and lifted a papilla preservation flap. Autogenous bone harvested from the upper jaw was used to fill in the defects in the lower jaw. The speaker also showed the final bridge which was created using CAD/CAM technology (Figures 19–22).
“We should avoid routine protocols. One case, one treatment plan.”
The speaker went on to discuss the high rate of complications (40%) associated with the all-on-implants approach. Although there is only short-term data available about them, monolithic zirconia prostheses may significantly reduce the rate of technical complications in full-arch implant rehabilitations (Kolgeci et al. 2014) compared with conventional metal-resin full-arch prostheses. Using two types of zirconia (tetragonal ZrO2 for the framework, and hexagonal ZrO2 for the teeth) may improve technical conditions without increasing costs.
Presentation figures

Figure 1
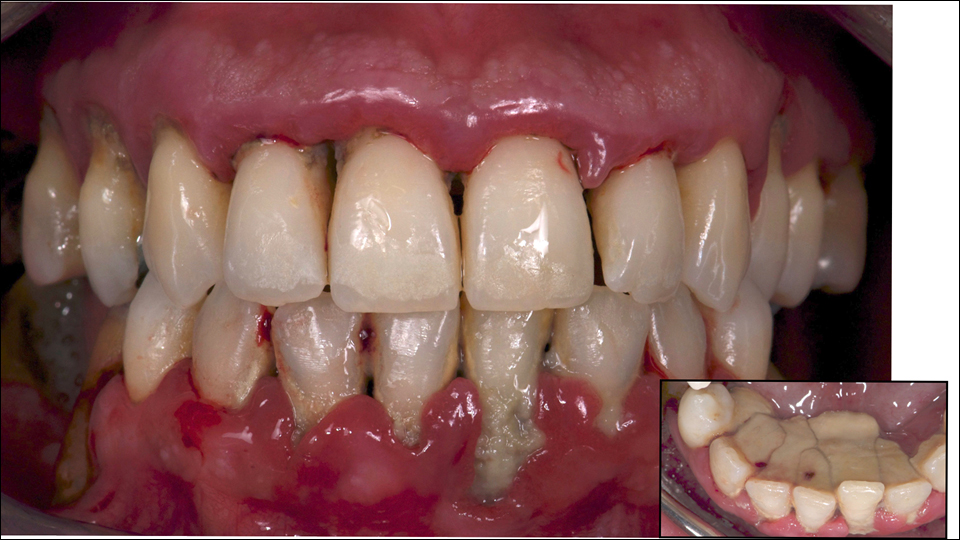
Figure 2

Figure 3
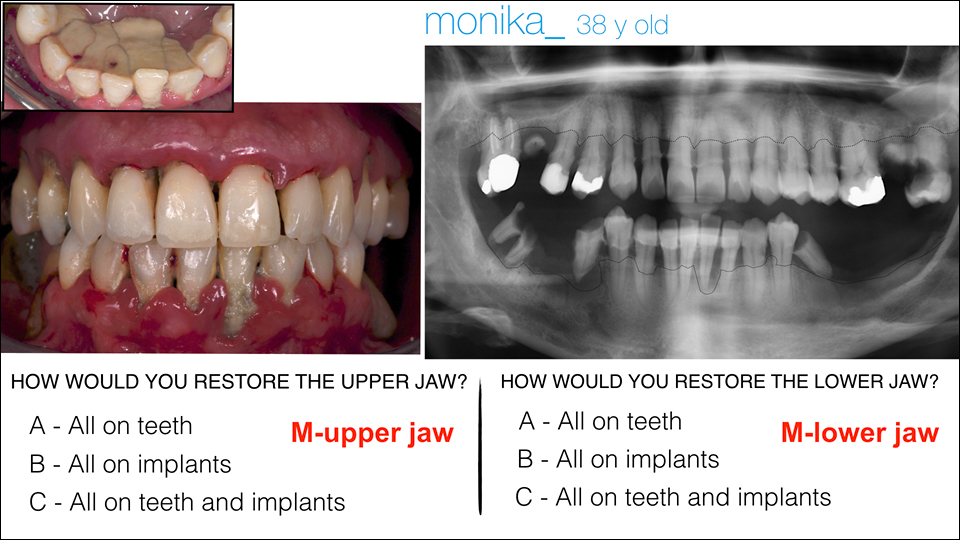
Figure 4
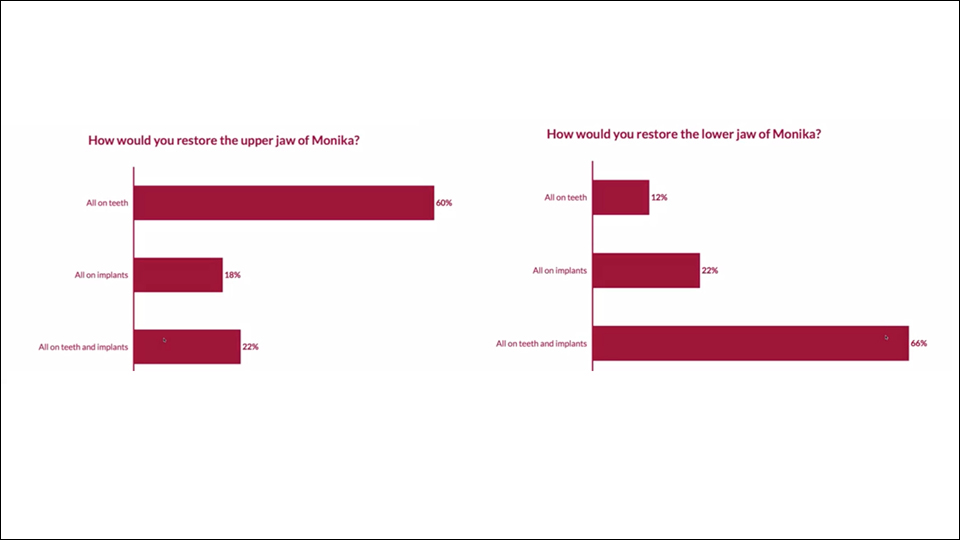
Figure 5
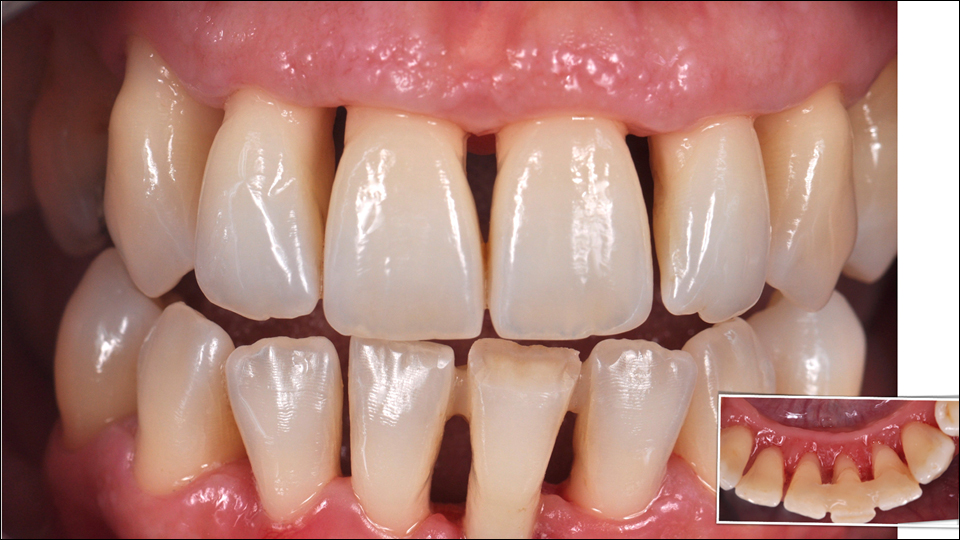
Figure 6

Figure 7
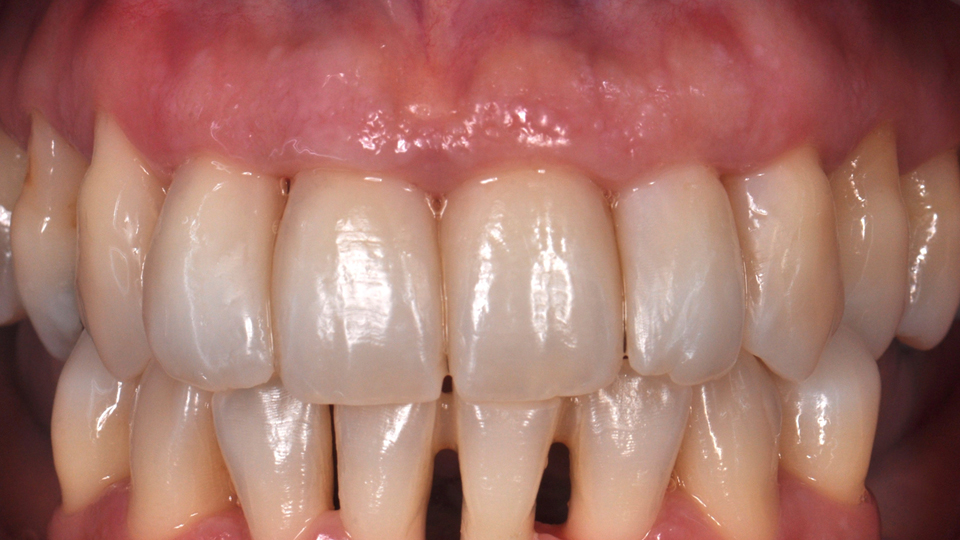
Figure 8
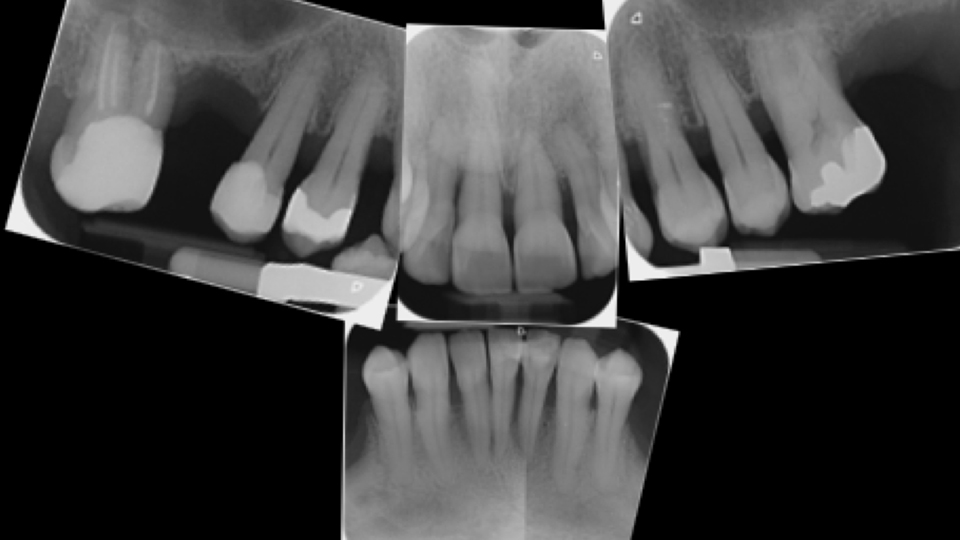
Figure 9

Figure 10

Figure 11
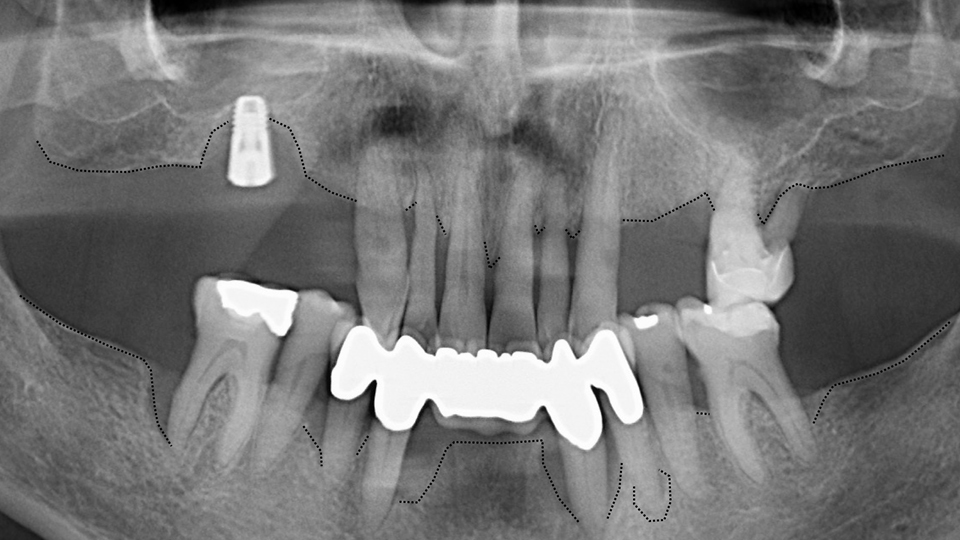
Figure 12
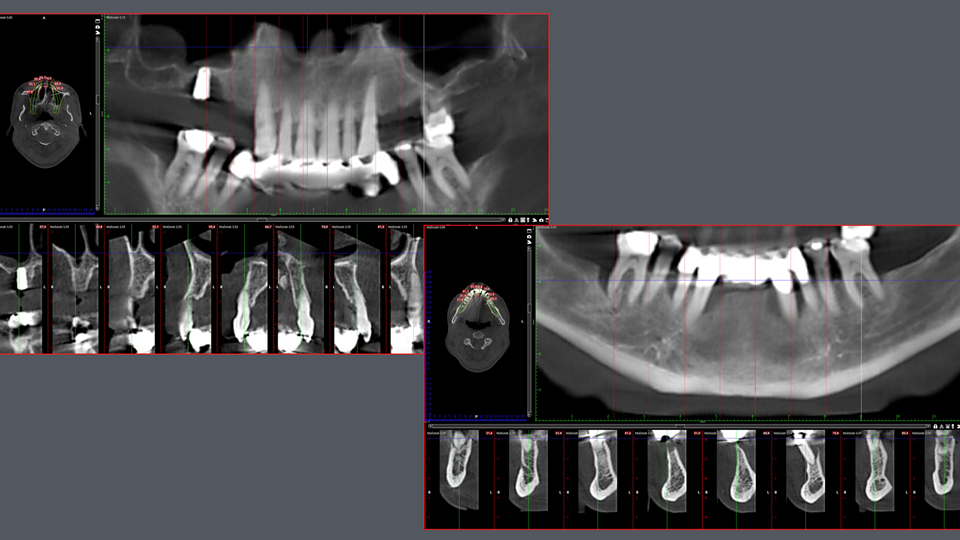
Figure 13
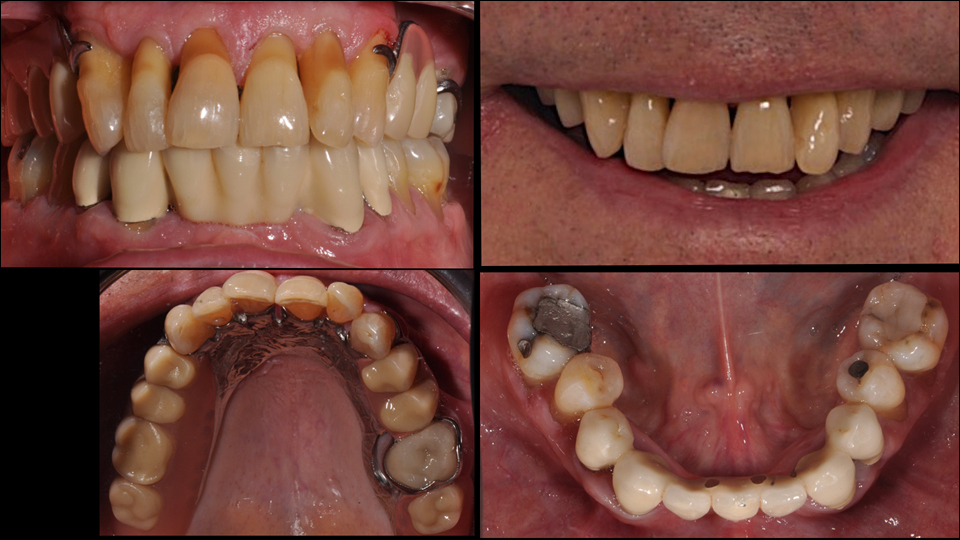
Figure 14
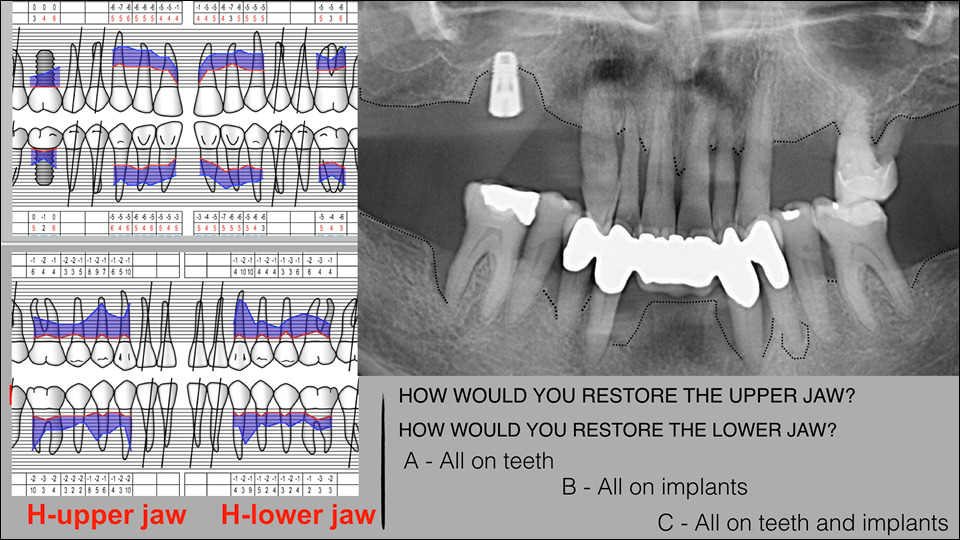
Figure 15
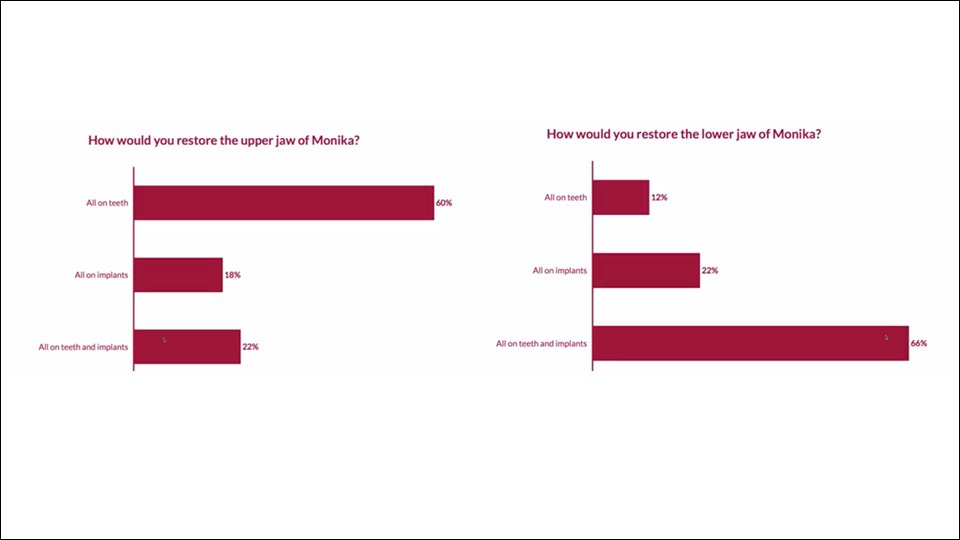
Figure 16

Figure 17

Figure 18
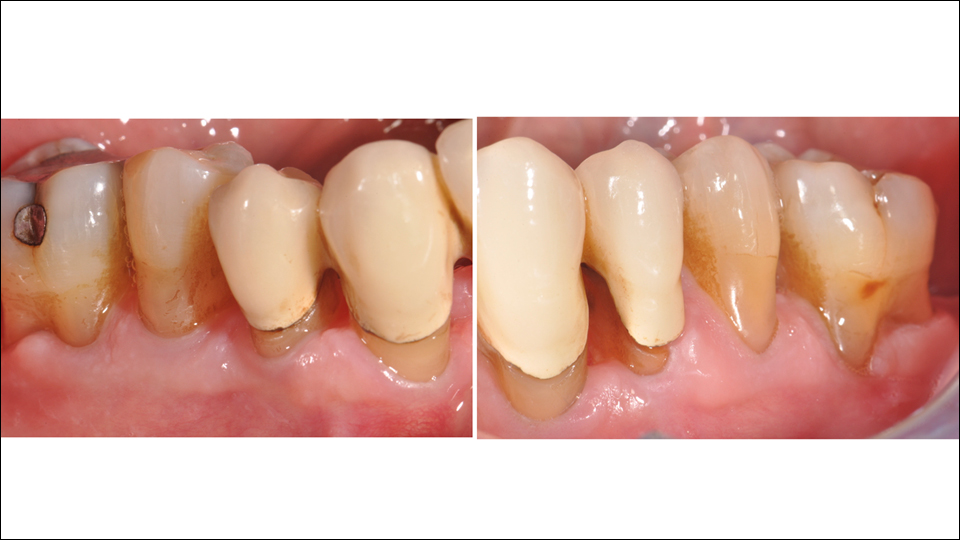
Figure 19
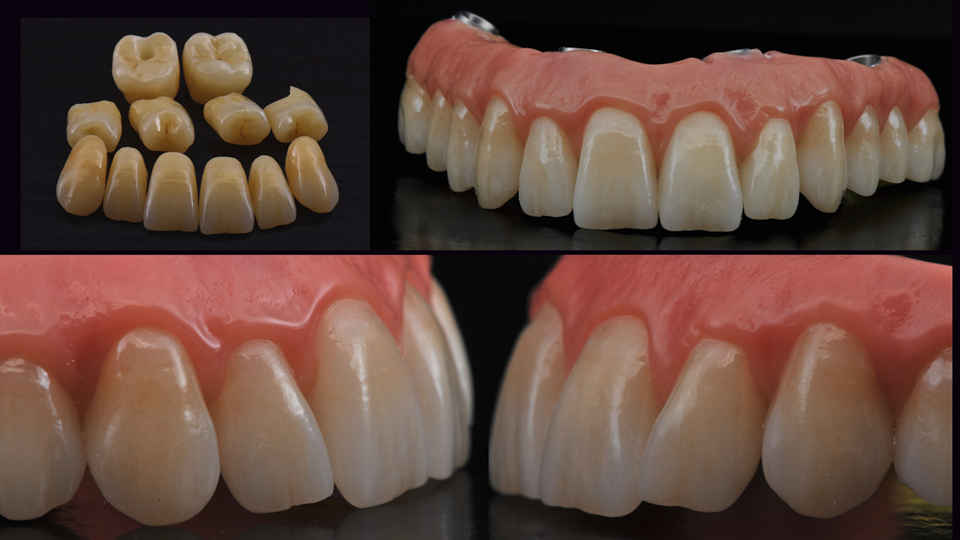
Figure 20
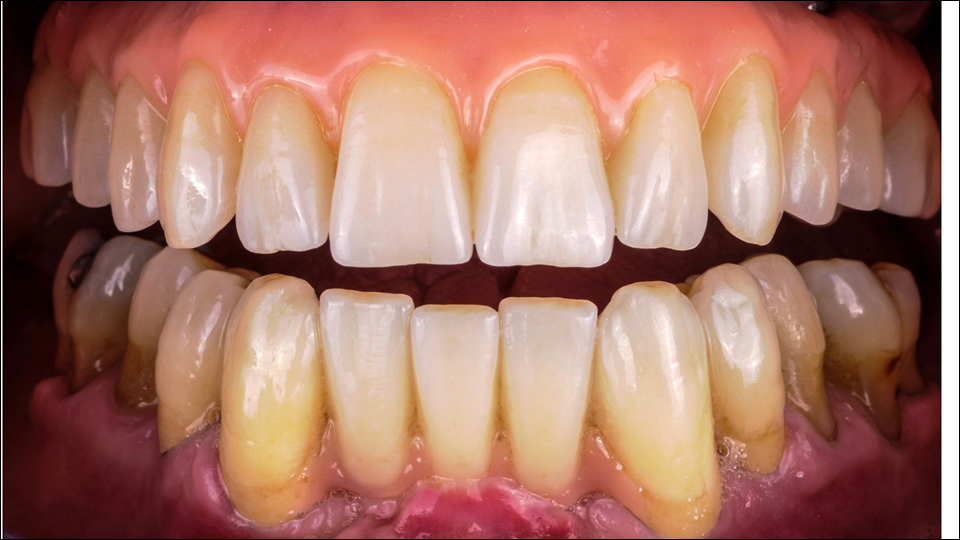
Figure 21
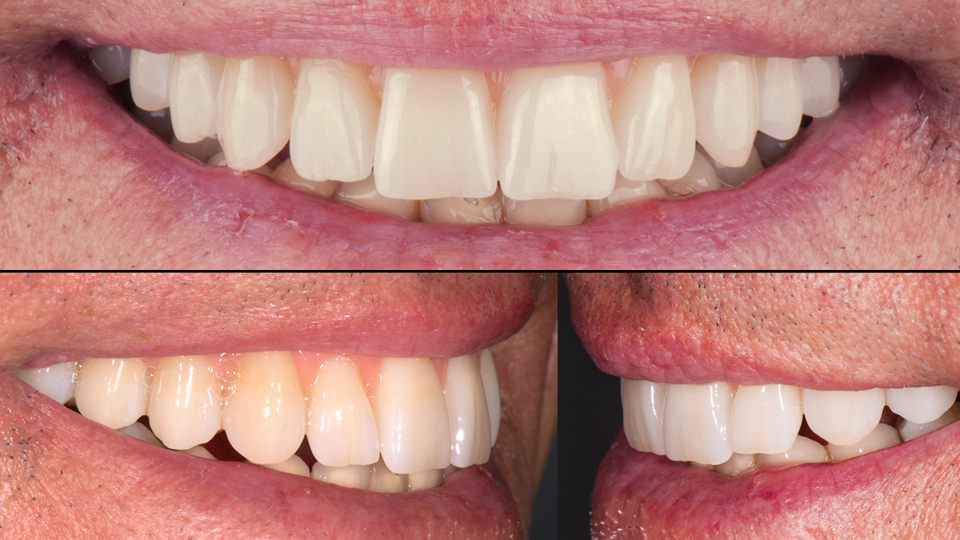
Figure 22
References:
Kolgeci L, Mericske E, Worni A, Walker P, Katsoulis J, Mericske-Stern R. Technical complications and failures of zirconia-based prostheses supported by implants followed up to 7 years: a case series. Int J Prosthodont. 2014 Nov-Dec;27(6):544–52. doi: 10.11607/ijp.3807.
Discussion
At several points during their case presentations, the speakers gave the audience the chance to vote on the treatment approach they would choose based on the information they were given. In all cases, the majority of the audience preferred to maintain at least some of the teeth and follow a combined ‘all-on-implants-and-teeth’ restoration. In the cases presented, it seemed preferable to keep the restorations separate (if possible) to avoid jeopardising the biomechanics by splinting ankylosed implants and periodontal teeth with mobility.
“The key factor in long-term success is not prosthodontic expertise but the ability to maintain periodontal health.”
The key factor in long-term success is not prosthodontic expertise but the ability to maintain periodontal health. Cleansability of the prosthesis is mandatory; maintenance is the key prognostic factor. The recall protocol should be completely tailored to the patient and the evolution of their periodontal parameters. The speakers also conceded that, while a combined ‘all-on-implants-and-teeth’ restoration may be the best all-round solution for the majority of cases, there are other times when the patient may want to prioritise aesthetics, or may have financial limitations. In these cases, an ‘all-on-implants’ approach may be more suitable, as a patient’s priorities should always be taken into account during the decision-making process.



